Urogynaecology
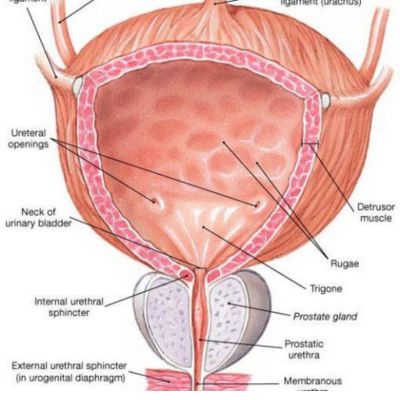
Urogynaecology
1) Recurrent urinary tract infections (UTI)
a. A UTI occurs when germs from outside the body enter the bladder, multiply and cause an infection. In some cases the germs will move up, out of the bladder and towards, or into, one or both of the kidneys.
b. Recurrent uncomplicated UTI may be defined as 3 or more uncomplicated UTIs in 12 months
c. Recurrent UTIs occur due to bacterial reinfection or bacterial persistence. Persistence involves the same bacteria not being eradicated in the urine 2 weeks after sensitivity-adjusted treatment. A reinfection is a recurrence with a different organism, the same organism in more than 2 weeks, or a sterile intervening culture (Level 4 evidence, Grade C recommendation).
Treatments and management
• Kidney or bladder stones
• Bacteria entering the urethra — the tube that carries urine from your body — during intercourse
• Changes in estrogen levels during menopause
• Abnormal urinary tract shape or function
Investigations
• Urine culture test of a sample obtained with a catheter
• Visual exam of the bladder and urethra with a lighted scope (cystoscopy)
Treatment is directed at the underlying cause, when possible. If your doctor can’t find a cause, one of these options may help:
• A long-term, low-dose antibiotic for as long as six months to two years
• Intermittent or post coital antibiotic therapy
• Vaginal estrogen therapy — if you don’t already take oral estrogen — for signs or symptoms related to vaginal dryness (atrophic vaginitis) after menopause
Life style changes
• Drink plenty of liquids, especially water, to help flush out bacteria
• Urinate often, especially when you feel the need
• Wipe from front to back after urination or a bowel movement
• Take showers rather than baths
• Gently wash the skin around your vagina and anus daily using a mild soap and plenty of water
• Use forms of birth control other than a diaphragm and spermicides
• Empty your bladder as soon as possible after intercourse
• Avoid deodorant sprays or scented feminine products in the genital area.
2) Pelvic organ prolapse
A bulge coming into the vagina. It can occur when there is a weakness in the muscles, ligaments or tissues of the pelvic floor which are supporting the uterus (womb) or vaginal walls. As a result the uterus or vaginal walls are not supported adequately, and may drop down causing a bulge to be felt or seen in the vagina.
Treatments and management
Depending on your prolapse, you may be considered for surgery.
3)Incontinence:
It is involuntary loss of urine which is objectively demonstrable and a social or hygiene problem”
Types of Incontinence :
• Stress Urinary Incontinence
• Urgency Incontinence:also known Overactive bladder (OAB)orDetrusor overactivity
• Mixed Incontinence-which has both stress and urge component
• Continuous Incontinence -occurs due to urinary fistulae
1)Stress incontinence
Leaking urine on activity such as coughing, sneezing, laughing or lifting. This may be caused by being overweight, or can appear after menopause, pregnancy or childbirth. You may be able to improve symptoms through weight loss, diet, stopping smoking and regular pelvic floor exercises.
Treatments and management
If lifestyle changes and pelvic floor exercises have not worked, we may recommend surgery (TransObturator tape-TOT insertion)to stabilise the urethra and reduce leakage.
2) Overactive bladder or Detrusor instability:
It is the feeling of need to empty your bladder too many times a day, for example, every hour or having to rush to empty your bladder.
The bladder holds 400 – 500mls of urine. An urge to pass urine is often felt when the bladder is half full in order to give you time to reach the toilet. Sometimes this message or urge may become blurred and your bladder will contract, wanting to empty without warning, leaving little time to reach the toilet.
Treatments and management
• Bladder retraining – this is the process whereby you retrain your bladder to hold a greater quantity of urine and should result in decreasing the frequency of urination. Try and avoid ‘just in case’ visits to the toilet.
• Fluid management – you are encouraged to drink 8-10 mugs a day to maintain tissue health and to keep your kidneys filtering. If you are tempted to cut down on your fluids to reduce frequency, then your urine will become more concentrated which will also irritate the bladder. Caffeine may be an irritant to your bladder, so it is a good idea to gradually reduce your intake of tea, coffee, high-energy drinks, and fizzy drinks.
• Medical treatment
3) Urinary Fistulas such as Vesicovaginal fistulas and ureterovaginal fistulas can result into continuous leakage. Treatment is usually surgery which is carried out typically 12 weeks after a prior surgery
Bladder Pain Syndrome
A feeling of discomfort or pain when the bladder is full and a frequent desire to empty the bladder.
What is urodynamics?
Urodynamic studies are performed to examine and assess the function and/or dysfunction of the lower urinary tract. Urinary assessment takes about 30-45 minutes to perform, and causes little discomfort. If cystoscopy is also performed the assessment takes approximately 60 minutes.
Urodynamic investigation usually includes :
• Urinary flow study (to assess urine flow rate, voided volume and voiding pattern)
• Bladder and perineal ultrasound (to assess residual urinary volume and urethral mobility)
• Cystometry (to assess bladder filling, storage and bladder pressures; to diagnose unstable bladder contractions)
• Urethral pressure profile (to measure maximal urethral pressure)
• Stress testing (to diagnose urodynamic stress incontinence)
Which patients should be referred for urodynamics?
• Patients with a complex picture of stress incontinence and urge incontinence.
• Women who have failed conservative treatment.
• Prior to surgery for stress incontinence.
• Women who have had previous continence surgery.
• Patients with symptoms of impaired bladder emptying.
• Prior to surgery for marked pelvic organ prolapse to exclude occult stress incontinence or impaired bladder emptying.
• Women with underlying neurological problems.
How is urodynamics performed ?
• Urodynamics is performed using computerised equipment and ultrasound imaging. The purpose of the examination is explained to the patient. The patient is asked to complete a bladder diary prior to urodynamics assessment. The patient is instructed to attend with a comfortably full bladder.
• The patient voids in private, into a toilet attached to a urodynamics computer. Initial flow rate and voided volume are recorded. Residual urine volume is measured by bladder ultrasonography. Measuring catheters are then inserted into the bladder and vagina(or rectum). These catheters are very fine (5-French) and generally do not cause the patient discomfort. All catheters used are disposable. Bladder and urethral pressures are calculated using water-perfused catheters that measure the change in intravesical pressure during bladder filling (cystometry). The bladder is filled with sterile water at room temperature at a constant rate (usually 80 mls per minute, but reduced if the patient presents with symptoms of urethral or bladder pain syndromes) to a maximum bladder volume of 500 mls.
• Urethral function is also assessed. The maximum urethral closure pressure is calculated. The calculation of this figure may influence the type of surgery recommended.
• At the end of the study voiding studies are repeated, to assess voiding efficiency and residual urinary volume. Voiding pressure is also measured to exclude bladder outlet obstruction.
• The results are then tabulated and urodynamics diagnosis made.
